The Evolution of Radiotherapy in India
Explore the historical journey of radiotherapy in India from 1910 to 2026. Understand how modern radiotherapy serves as a primary tool for cancer treatment, debunk myths, and learn about organ preservation. Gain insights into India's cancer care infrastructure and practical advice for patients.
GENERAL INFORMATION

Radiation therapy (radiotherapy) often sounds frightening. Many people imagine “burns”, “damage”, or something new and experimental. In reality, radiotherapy has been part of India’s cancer care story for more than a century — quietly treating millions of patients.
Using the best available national data and published research, a conservative estimate suggests that around 10–12 million people in India have received radiotherapy between 1910 and 2026 (Mehta, Indian J Surg Oncol, 2022; Sathishkumar et al., Indian J Med Res, 2023; Chauhan et al., J Med Phys, 2024; Soni et al., Rep Pract Oncol Radiother, 2025).
1. Why is it hard to know the exact number?
There is no single official national registry that has counted every radiotherapy patient since the beginning of the specialty in India. Early records were paper‑based, kept locally, and often incomplete.
So instead of one master list, experts combine:
Historical hospital reports from major centers
Modern cancer registry data (National Cancer Registry Programme, ICMR)
Recent infrastructure studies on how many radiotherapy machines and centers exist, and how many patients they treat (Chauhan et al., J Med Phys, 2024; Soni et al., Rep Pract Oncol Radiother, 2025)
Published estimates of how many cancer patients typically need radiotherapy (Abdel‑Wahab et al., Clin Oncol, 2017)
From these, a reasoned, conservative estimate is built. Whenever the evidence is uncertain, the numbers below lean on the safer, lower side.
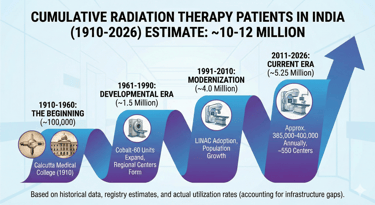
2. The big picture: 10–12 million Indians treated with radiotherapy
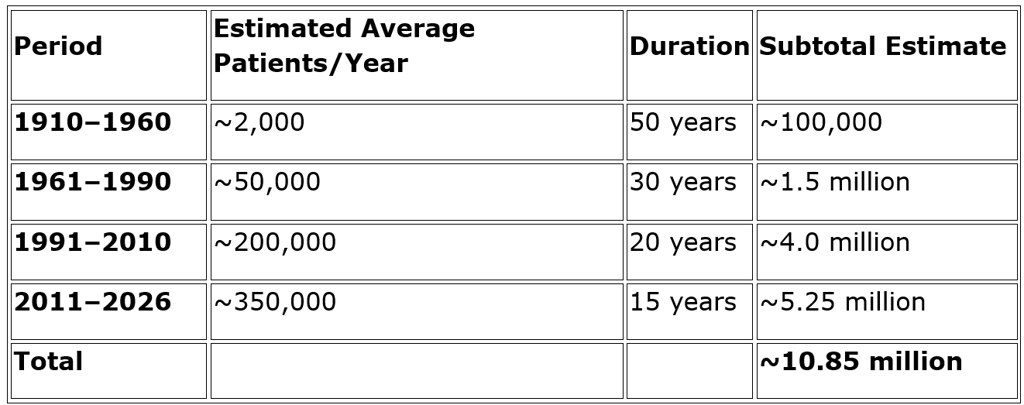
Putting all periods together, the best current estimate is:
Total Indians treated with radiotherapy (1910–2026): ~10.8 million (range ~10–12 million)
This is based on reconstructed annual treatment volumes, cancer incidence, and realistic utilization of existing machines over time (Mehta, 2022; Sathishkumar et al., 2023; Chauhan et al., 2024; Soni et al., 2025).
Approximate breakdown by era
These are conservative numbers, adjusted for the fact that many patients who needed radiotherapy in the past never received it because of shortages of machines, centers, or specialists (Chauhan et al., 2024).
If India had always met international recommendations for radiotherapy access, the true number of treated patients could easily have been almost double (Abdel‑Wahab et al., Clin Oncol, 2017).
3. The modern era (2000–today): where most treatments happened
The last 20–25 years have seen a sharp rise in cancer cases and a rapid expansion of radiotherapy services.
New cancer cases: About 1.46 million new cancer cases were estimated in India in 2022 (Sathishkumar et al., 2023).
How many should get radiotherapy? Globally, about 50–60% of cancer patients need radiotherapy at least once in their lifetime (Abdel‑Wahab et al., 2017). That would mean roughly 800,000–850,000 Indians per year ideally needing radiotherapy in 2022.
How many actually receive it? Analyses of actual Indian data suggest that only about 28.5% of cancer patients received radiotherapy in 2022 — around 385,000–400,000 patients (derived from Sathishkumar et al., 2023; utilization assumptions consistent with Chauhan et al., 2024).
So today:
Optimal need: ~58% of cancer patients (Abdel‑Wahab et al., 2017)
Actual Indian utilization: ~28.5% (Sathishkumar et al., 2023 + derived RT use estimates)
This gap is what experts call the “radiotherapy utilization gap” — patients who should receive radiotherapy but do not.
Current annual volume (approx.)
2022–2024: ~385,000–400,000 patients/year receiving radiotherapy in India
(Sathishkumar et al., 2023; Chauhan et al., 2024; Soni et al., 2025)
Over 15 years (2011–2026), even using a cautious average of ~350,000 treatments per year, this gives approximately 5.25 million radiotherapy treatment courses in this period alone.
4. How many centers and machines does India have?
Reliable 2022 national data show (Chauhan et al., J Med Phys, 2024):
Radiotherapy centers (institutes): 554
Teletherapy machines (external beam radiotherapy): 823
~624 linear accelerators (linacs) – modern, precise machines
~151 telecobalt machines – older, cobalt‑60 based units
~48 other advanced machines like Gamma Knife, CyberKnife, Tomotherapy
On average:
1.5 machines per center, but
69.4% of centers have only one machine (Chauhan et al., 2024)
This means many centers have very limited capacity. If that one machine is under maintenance or breaks down, treatment can be delayed.
Machine density – how far are we from ideal?
Using 2016 cancer incidence and projected 2022 need, the same study found (Chauhan et al., 2024):
Estimated radiotherapy patients in 2022: ~0.92 million
Recommended: 1 teletherapy machine per 450 radiotherapy patients (IAEA standard; Abdel‑Wahab et al., 2017)
Machines needed for India in 2022: ~2,049
Machines actually available: 823
Shortfall: ~1,200 machines
Expressed per population:
Current machine density (2022): ~0.6 machines per million people
Required density for India’s need: ~1.5 machines per million people
(Chauhan et al., 2024)
In simple terms: India has only about 40% of the radiotherapy machines it needs for its population and cancer burden.
5. The historical journey: from X‑ray rooms to modern linacs
a) The very early years (1910–1950)
First X‑ray therapy facility in India:
Calcutta Medical College, 1910 (Mehta, Indian J Surg Oncol, 2022).Other early centers:
Government X‑ray Institute, Chennai (1924)
Patna Radium Institute (1927) (Mehta, 2022)
In this era:
Equipment was basic.
Cancer diagnosis itself was far less common.
Total treated patients across India in these 40 years are estimated at under 100,000.
Even large centers like Tata Memorial Hospital were still growing into their role.
b) The developmental era (1950–1999)
This is when radiotherapy started becoming more widely available, especially in big cities.
1941–1950: Tata Memorial Hospital (Mumbai) treated about 10,000 patients with deep X‑ray therapy in that decade (~1,000 per year) (Mehta, 2022).
1965: only 19 institutions with telecobalt units in the entire country (Mehta, 2022).
1978: this had grown to 63 radiotherapy departments (Mehta, 2022).
Still, total national volume remained modest by today’s standards, because:
Machines were fewer and slower.
Travel was difficult; radiotherapy was concentrated in metros.
Awareness and diagnosis rates were lower.
A realistic reconstruction suggests:
1961–1990: about 50,000 patients per year on average,
totaling around 1.5 million over 30 years.
c) The transition to the modern linac era (2000–2022)
Over the last 22 years, two important changes occurred (Chauhan et al., 2024):
Number of machines increased, especially linacs.
Share of advanced technology rose sharply:
In 2000, linacs were only 12.2% of all RT machines.
By 2010, they were 43.1%.
By 2022, linacs were 75.8% of all machines.
Telecobalt machines, once the workhorse of Indian radiotherapy, have steadily decreased, though many are still in use, especially in lower‑resource regions (Chauhan et al., 2024).
6. Unequal access inside India: where you live still matters
The distribution of radiotherapy in India is not uniform (Chauhan et al., 2024):
Southern India has the highest share of centers and machines:
~35% of radiotherapy centers
~34.5% of machines
North‑Eastern India has the lowest:
~4.5% of centers and machines
By states:
Highest number of centers and machines:
Maharashtra, Tamil Nadu, Uttar Pradesh (Chauhan et al., 2024)
Highest machine density (machines per million people):
Puducherry (~2.94 machines/million)
Delhi (~2.05 machines/million)
Mizoram (~1.63 machines/million)
Lowest machine density:
Bihar (~0.08 machines/million)
Jharkhand (~0.18 machines/million)
Uttar Pradesh (~0.25 machines/million) (Chauhan et al., 2024)
This means that two patients with the same cancer may have very different radiotherapy access purely based on which state they live in.
7. What does this mean for patients and families?
1) Radiotherapy is not rare or experimental in India
With around 10–12 million Indians treated since 1910, radiotherapy is one of the most widely used and studied cancer treatments in the country (Mehta, 2022; Chauhan et al., 2024). It is a standard, evidence‑based part of care for breast, head‑and‑neck, cervical, prostate, brain, lung and many other cancers (Abdel‑Wahab et al., 2017).
2) The real problem is access and capacity, and lack of awareness. Not safety.
The main concern in India is too few machines and centers for the number of patients who need them (Chauhan et al., 2024).
This leads to:
Long travel distances
Waiting lists
Patients dropping out of treatment due to cost, logistics or fatigue
Radiotherapy itself, when properly planned and delivered, is safe, precise and highly regulated, with strong national and international quality and safety standards (IAEA; Abdel‑Wahab et al., 2017).
3) Modern technology is already here — but not everywhere
Many major centers now use advanced linear accelerators, image‑guided and intensity‑modulated radiotherapy, and stereotactic techniques (Chauhan et al., 2024; Soni et al., 2025).
Some centers have Gamma Knife and CyberKnife for brain and selected body lesions (Chauhan et al., 2024).
However, these are still concentrated in urban, better‑resourced regions.
8. If you or a loved one is facing cancer: what should you ask?
“Is radiotherapy part of the standard treatment for my type and stage of cancer?”
Ask whether the goal is cure, organ preservation, or symptom relief.
“Where is the nearest center with appropriate technology for my case?”
In some situations, travelling a bit farther for a better‑equipped center can matter.
“What are the waiting times and how will that affect my outcome?”
In many cancers, timely radiotherapy is important.
“What support exists for travel, accommodation or government schemes?”
Different states and central schemes may help with costs; hospital social work teams can guide you.
“Can you explain my treatment plan in simple language?”
You have the right to clear, jargon‑free explanations.
6. “Where can I meet a radiation Oncologist to understand his perspective?
o You have the right to know less toxic and less invasive modern options too.
9. Key take‑home messages
Radiotherapy has been used in India for over 100 years, with the first facility starting in 1910 at Calcutta Medical College (Mehta, 2022).
A careful combination of cancer registry data and infrastructure studies suggests that around 10–12 million Indians have received radiotherapy between 1910 and 2026.
Most of these treatments (over 80–90%) happened in the last 30–35 years, as cancer incidence rose and facilities expanded (Mehta, 2022; Sathishkumar et al., 2023; Chauhan et al., 2024).
India currently has 823 radiotherapy machines across 554 centers, but needs roughly 2,000+ machines to meet its true cancer burden (Chauhan et al., 2024).
Machine density is only about 0.6 per million people, versus an estimated need of ~1.5 per million (Chauhan et al., 2024; Abdel‑Wahab et al., 2017).
Where you live still strongly influences your access — southern and some union territories are better served than large states like Bihar and Uttar Pradesh (Chauhan et al., 2024).
Radiotherapy itself is not an experimental treatment. It is a standard, globally accepted cancer cure therapy with decades of safety protocols behind it (Abdel‑Wahab et al., 2017).
The main challenge for India is expanding fair access — more machines, more aware healthcare professionals, more trained staff, and better geographic distribution — not whether radiotherapy works.
Keep in mind:
No one can provide an exact, named‑patient count from 1910 to 2026.
Early‑period estimates (1910–1960) are particularly uncertain and rely on historical reconstruction (Mehta, 2022).
However, even with conservative assumptions, every robust analysis arrives in the 10+ million range for cumulative Indian radiotherapy treatments when extrapolated over 100+ years using national cancer incidence and modern utilization data (Sathishkumar et al., 2023; Chauhan et al., 2024; Soni et al., 2025).
References
Mehta A. Tracking the Development of Cancer Care After 75 Years of Independence: India’s Fight Against Cancer Since 1947. Indian J Surg Oncol. 2022;13(1):12‑26. doi:10.1007/s13193‑022‑01689‑2.
Sathishkumar K, Chaturvedi M, Das P, Stephen S, Mathur P. Cancer incidence estimates for 2022 & projection for 2025: Result from National Cancer Registry Programme, India. Indian J Med Res. 2023;156(4‑5):598‑607. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC10231735/.
Chauhan RS, Munshi A, Pradhan A. An Analysis of Radiotherapy Machine Requirements in India: Impact of the Pandemic and Regional Disparities. J Med Phys. 2024;49(3):370‑378. doi:10.4103/jmp.jmp_20_24. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC11548067/.
Soni P, Kaushal V, Verma M. Establishing a radiation oncology department in India: key challenges and essential considerations from the perspective of radiation oncology professionals. Rep Pract Oncol Radiother. 2025. Available at: https://journals.viamedica.pl/rpor/article/view/104386/82459.
Abdel‑Wahab M, Fidarova E, Polo A. Global Access to Radiotherapy in Low‑ and Middle‑income Countries. Clin Oncol (R Coll Radiol). 2017;29(2):99‑104. doi:10.1016/j.clon.2016.12.004. Available at: https://pubmed.ncbi.nlm.nih.gov/28040092/.